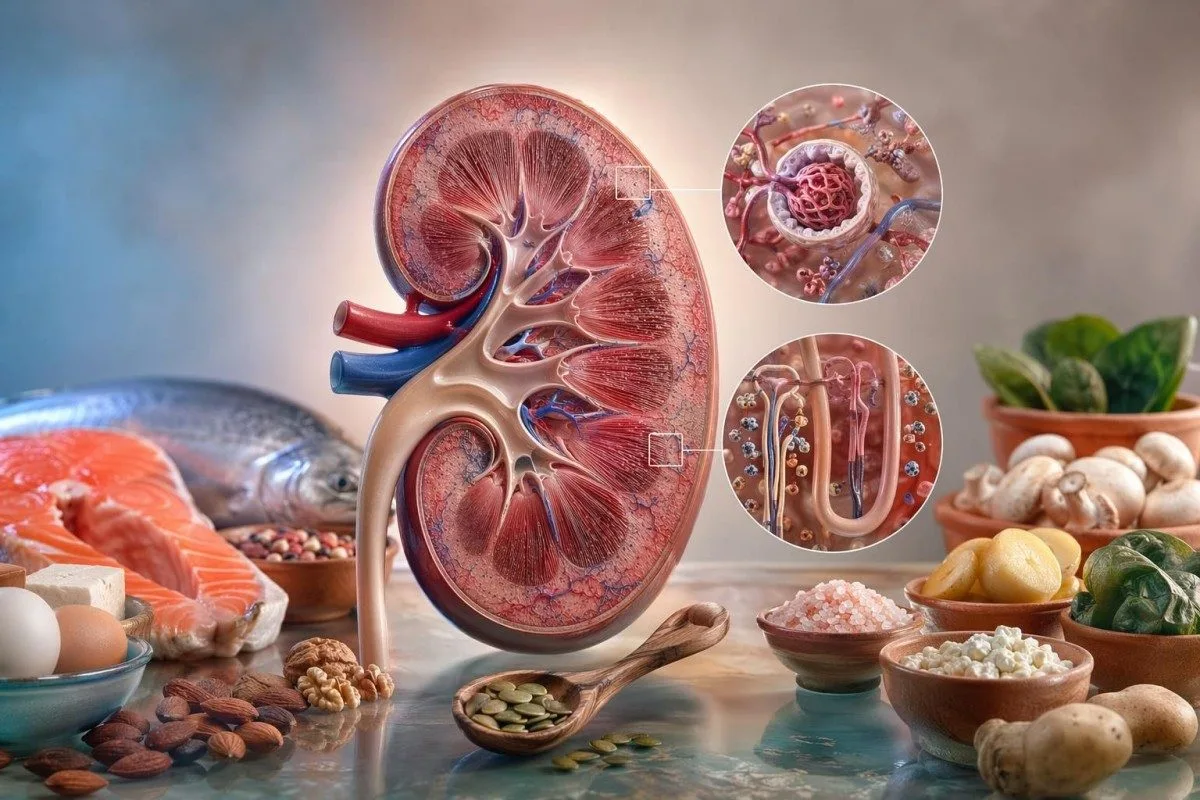
Kidney nutrition is not a single food list. Your safest choices depend on eGFR, urine albumin, potassium, bicarbonate, phosphate, blood pressure, medicines and what your previous labs were already doing.
This guide was written under the leadership of Dr. Thomas Klein, MD in collaboration with the Kantesti AI Medical Advisory Board, including contributions from Prof. Dr. Hans Weber and medical review by Dr. Sarah Mitchell, MD, PhD.

Thomas Klein, MD
Chief Medical Officer, Kantesti AI
Dr. Thomas Klein is a board-certified clinical hematologist and internist with over 15 years of experience in laboratory medicine and AI-assisted clinical analysis. As Chief Medical Officer at Kantesti AI, he leads clinical validation processes and oversees the medical accuracy of our 2.78 trillion parameter neural network. Dr. Klein has published extensively on biomarker interpretation and laboratory diagnostics in peer-reviewed medical journals.

Sarah Mitchell, MD, PhD
Chief Medical Advisor - Clinical Pathology & Internal Medicine
Dr. Sarah Mitchell is a board-certified clinical pathologist with over 18 years of experience in laboratory medicine and diagnostic analysis. She holds specialty certifications in clinical chemistry and has published extensively on biomarker panels and laboratory analysis in clinical practice.

Prof. Dr. Hans Weber, PhD
Professor of Laboratory Medicine & Clinical Biochemistry
Prof. Dr. Hans Weber brings 30+ years of expertise in clinical biochemistry, laboratory medicine, and biomarker research. Former President of the German Society for Clinical Chemistry, he specializes in diagnostic panel analysis, biomarker standardization, and AI-assisted laboratory medicine.
- eGFR below 60 mL/min/1.73 m² for more than 3 months suggests chronic kidney disease, especially when urine ACR is 30 mg/g or higher.
- BUN commonly runs 7–20 mg/dL in adults; a rise after high-protein eating can happen without a matching creatinine rise.
- Creatinine can increase after cooked meat, creatine supplements, dehydration, heavy training or trimethoprim, so trends matter more than one value.
- Sodium under about 2,000 mg/day is often advised for CKD with high blood pressure, but athletes, low-sodium patients and some older adults need caution.
- Potassium usually measures 3.5–5.0 mmol/L; foods high in potassium are not automatically banned unless labs, medicines or eGFR make retention likely.
- Phosphorus is more dangerous from additives than from beans or nuts because additive phosphorus may be absorbed at 90–100%.
- Magnesium is often 1.7–2.2 mg/dL; foods high in magnesium can help metabolic health, but supplements may be risky in advanced CKD.
- Urine albumin-creatinine ratio below 30 mg/g is usually normal, 30–300 mg/g is moderately increased, and above 300 mg/g signals higher kidney and cardiovascular risk.
The safest kidney diet starts with your actual lab pattern
A good diet for kidney disease protects labs by matching protein, sodium, potassium and phosphorus to your eGFR, urine protein, electrolytes and medicines—not by banning the same foods for everyone. If potassium is 4.2 mmol/L, phosphate is 3.6 mg/dL and urine ACR is high, I often worry more about sodium and blood pressure than about a banana.

I’m Thomas Klein, MD, and when I review kidney panels in Kantesti AI, the first question is not “what food is bad?” It is whether the pattern looks like filtration loss, dehydration, medication effect, protein spill, acid load, mineral imbalance or simply a noisy single result; our diet for kidney disease interpretation starts there.
As of April 29, 2026, KDIGO defines chronic kidney disease by abnormalities of kidney structure or function present for at least 3 months, including eGFR below 60 mL/min/1.73 m² or urine ACR of 30 mg/g or higher (KDIGO, 2024). That time requirement matters; I have seen anxious patients overhaul their whole diet after one post-gym creatinine result that normalized 10 days later.
One useful frame: diet rarely “raises eGFR” directly in a week, but it can move risk markers around eGFR. Sodium can change blood pressure and albuminuria, protein can shift BUN, cooked meat can nudge creatinine, potassium intake can expose impaired excretion, and phosphorus additives can push PTH long before a patient feels anything.
For background on age-related filtration and why a single estimate can mislead, our eGFR age guide is a good companion read. The practical move is to compare your current panel with prior creatinine, cystatin C if available, ACR, CO2, potassium, phosphate and blood pressure—not to follow a photocopied kidney diet from a waiting room.
eGFR, creatinine and cystatin C tell different nutrition stories
eGFR estimates filtration, while creatinine and cystatin C are the ingredients used to estimate it. Creatinine is strongly affected by muscle mass, meat intake and some medicines, whereas cystatin C is less tied to muscle but can shift with inflammation, steroid use and thyroid status.

A creatinine-based eGFR of 58 mL/min/1.73 m² does not mean the same thing in a 32-year-old bodybuilder as it does in an 82-year-old with weight loss. Kantesti AI compares creatinine, body context, BUN, electrolytes and historical results using our clinical validation standards rather than treating the flag as the diagnosis.
Serum creatinine is commonly about 0.6–1.1 mg/dL in adult women and 0.7–1.3 mg/dL in adult men, but lab ranges vary by method and population. Some European labs report creatinine in µmol/L, where 1.0 mg/dL is approximately 88.4 µmol/L, and unit mix-ups are more common than patients think.
Cystatin C can be useful when creatinine looks out of proportion to the person in front of us. A frail patient with “normal” creatinine of 0.9 mg/dL may still have low true filtration, while a muscular patient with creatinine of 1.4 mg/dL may have a more reassuring cystatin C-based eGFR.
When eGFR and creatinine disagree, look for diet timing before assuming decline. Our guide to a low GFR with normal creatinine explains why equations can mislead at the edges of age, muscle mass and body size.
Protein changes BUN faster than it changes eGFR
Protein intake most directly affects BUN, not eGFR. BUN commonly ranges from 7–20 mg/dL in adults, and a rise after a high-protein week can reflect urea production rather than sudden kidney injury.

KDOQI’s 2020 nutrition guideline recommends individualized protein targets, including about 0.55–0.60 g/kg/day for metabolically stable adults with CKD stages 3–5 without diabetes when supervised, and 0.6–0.8 g/kg/day for many adults with diabetes and CKD (Ikizler et al., 2020). Dialysis is different; many dialysis patients need roughly 1.0–1.2 g/kg/day because treatment increases amino acid losses.
I see this pattern all the time: a patient starts 140 g/day of protein powder, BUN rises from 16 to 31 mg/dL, creatinine barely moves, and urine ACR is unchanged. That pattern is not the same as a falling eGFR, but it is a signal to ask whether the protein target fits kidney stage, body weight, training load and appetite.
A BUN-creatinine ratio above 20:1 often suggests dehydration, high protein intake, gastrointestinal nitrogen load or reduced kidney perfusion rather than intrinsic kidney damage by itself. Our BUN interpretation guide goes deeper into why BUN is a noisy marker when read alone.
A safer protein adjustment is usually gradual: trim excess powders first, spread protein across meals, and avoid dropping below what prevents muscle loss. In older adults, I am cautious about aggressive restriction because sarcopenia can lower creatinine and make eGFR look deceptively better.
Creatinine can rise from meat, creatine and hard training
Creatinine can rise for reasons that have little to do with permanent kidney damage. Cooked meat, creatine supplements, dehydration, heavy resistance exercise and medicines such as trimethoprim can all raise creatinine or lower calculated eGFR temporarily.

A 41-year-old cyclist once uploaded a panel after a weekend race: creatinine 1.38 mg/dL, eGFR 61 mL/min/1.73 m², BUN 28 mg/dL and CK mildly high. Three days of hydration and no hard training brought creatinine back to 1.08 mg/dL; that is why context beats panic.
Creatinine is produced from muscle creatine, so higher muscle mass and recent muscle breakdown can increase the result. The cleanest repeat test is often after 24–48 hours without intense exercise and without a large cooked-meat meal the night before, especially if the result will decide a referral.
Creatine monohydrate is not automatically kidney-toxic in healthy adults, but in CKD it complicates interpretation because it can increase creatinine generation. If your eGFR is already borderline, our creatinine range guide explains when cystatin C or a urine ACR may clarify the story.
Do not “water-load” aggressively before a repeat panel. Overhydration can dilute sodium and albumin, while ordinary hydration—clear to pale-yellow urine, no vomiting or diarrhoea—is usually enough for a fair kidney chemistry test.
Sodium affects kidney risk through pressure and urine protein
Sodium is one of the most lab-relevant diet changes in CKD because it can lower blood pressure and reduce urine albumin. Serum sodium usually stays 135–145 mmol/L, so the kidney benefit is often seen in blood pressure and ACR rather than the sodium blood result itself.

KDIGO and many nephrology clinics commonly aim for sodium intake below about 2,000 mg/day in CKD patients with hypertension, though frail older adults, heavy sweaters and people with low sodium need individual advice. A low-salt diet that causes dizziness, falls or sodium of 130 mmol/L is not a win.
The DASH diet for blood pressure is powerful, but kidney patients may need a modified version because standard DASH is rich in potassium and phosphorus-containing foods. In the DASH-Sodium trial, the combination of DASH eating and low sodium lowered systolic blood pressure by about 7.1 mmHg in non-hypertensive adults and 11.5 mmHg in hypertensive adults compared with a high-sodium control diet (Sacks et al., 2001).
Albuminuria is where sodium gets interesting. When sodium intake is high, ACE inhibitors and ARBs often reduce urine protein less effectively; when sodium falls, the same medication can look more potent on the next ACR.
If your home readings are high, compare them with standardized technique before blaming dinner. Our blood pressure range guide explains why cuff size, rest time and morning medication timing can change the number by 10 mmHg.
Foods high in potassium are not automatically forbidden
Foods high in potassium only need restriction when your lab pattern shows potassium retention risk. A potassium of 3.8 mmol/L on a thiazide diuretic is a different problem from 5.7 mmol/L on spironolactone with eGFR 28.
Serum potassium usually ranges from 3.5–5.0 mmol/L, and values above 5.5 mmol/L generally deserve prompt review. A result of 6.0 mmol/L or higher can be urgent, especially with weakness, palpitations, ECG changes, advanced CKD or potassium-raising medicines.
Common foods high in potassium include bananas, oranges, potatoes, tomatoes, spinach, avocado, dried fruit, beans and coconut water. The catch: potassium from whole plants is often less completely absorbed than potassium salts in supplements, low-sodium salt substitutes and processed foods.
I have seen patients remove nearly every fruit and vegetable after one potassium of 5.2 mmol/L, then return constipated, acidotic and miserable. Before doing that, check for hemolysis on the sample, recent medication changes, salt substitutes, trimethoprim, NSAIDs, ACE inhibitors, ARBs, spironolactone and whether the blood draw was difficult.
For patients who truly need lowering, portion size and cooking method help. Our potassium range guide covers leaching potatoes, avoiding potassium chloride salts and watching the trend after changes.
Potassium, CO2 and chloride explain more together
Kidney diet decisions are safer when potassium is read with CO2, chloride and sodium. Low CO2 can suggest metabolic acidosis, which changes protein tolerance, bone-mineral risk and how much plant food a patient can safely use.

Serum CO2 on a basic metabolic panel usually reflects bicarbonate and often ranges from 22–29 mmol/L. In CKD, a CO2 below 22 mmol/L can suggest metabolic acidosis, which is linked with muscle loss, bone buffering and faster kidney decline in some cohorts.
Here is a pattern I do not ignore: potassium 5.3 mmol/L, chloride 111 mmol/L, CO2 18 mmol/L and eGFR 34 mL/min/1.73 m². That combination can make a high-fruit “alkaline” diet attractive in theory, but the potassium risk means a clinician may consider bicarbonate therapy, medication review or carefully selected lower-potassium produce instead.
Kantesti’s neural network groups electrolytes into patterns rather than reading them as isolated flags. If you want the basics first, our electrolyte panel guide explains how sodium, potassium, chloride and CO2 point toward dehydration, acid-base disorders or medication effects.
Do not use baking soda on your own if you have high blood pressure, swelling or heart failure. One teaspoon contains roughly 1,200 mg of sodium, enough to undo a careful low-sodium kidney plan.
Foods high in magnesium can help, but supplements need respect
Foods high in magnesium are usually safer than magnesium supplements in CKD, but advanced kidney disease changes the margin. Serum magnesium commonly measures 1.7–2.2 mg/dL, and levels above about 2.6 mg/dL suggest retention or excess intake in many labs.

Magnesium-rich foods include pumpkin seeds, almonds, cashews, beans, lentils, spinach, dark chocolate and whole grains. Those same foods may also contain potassium or phosphorus, so the right serving depends on phosphate, potassium, bowel habits, diabetes status and eGFR stage.
The evidence around magnesium and CKD is honestly mixed. Low magnesium is associated with insulin resistance, arrhythmia risk and vascular calcification in observational work, but supplements can accumulate when eGFR is low, especially with magnesium-containing laxatives or antacids.
I am much more comfortable with food-first magnesium when potassium is normal and phosphate is controlled. Our magnesium range guide explains why a “normal” serum magnesium can still miss intracellular depletion, particularly in people taking PPIs or loop diuretics.
A practical checkpoint: if eGFR is below 30 mL/min/1.73 m², ask before taking magnesium glycinate, citrate or oxide. Magnesium toxicity can cause low blood pressure, sluggish reflexes, sleepiness and rhythm problems when levels climb substantially.
Phosphorus additives move labs more than beans do
Phosphorus from additives is usually more lab-disruptive than phosphorus naturally trapped in plant foods. Serum phosphorus is commonly 2.5–4.5 mg/dL, but PTH and FGF23 may rise before phosphorus leaves the reference range.

This is the part patients rarely hear: phosphorus in cola drinks, processed meats, shelf-stable baked goods and “enhanced” packaged foods may be absorbed at 90–100%, while plant phytate phosphorus is often absorbed far less. So a bean stew and a processed phosphate-added meal can have very different lab effects even if the label looks similar.
High phosphorus in CKD links to secondary hyperparathyroidism, vascular calcification risk and bone turnover problems. A PTH result drifting upward with normal calcium and phosphorus may be an early mineral-bone clue, not a reason to randomly cut all protein.
Food labels are frustrating because phosphorus milligrams are not always listed. Look for ingredient words containing “phos,” and pair that with your renal panel; our PTH blood test guide explains how calcium, vitamin D, phosphate and PTH fit together.
I often ask patients to remove phosphate additives for 4–6 weeks before we cut healthy whole foods. That single change can lower phosphate burden without worsening fibre intake, constipation, cholesterol or glucose control.
Urine protein often responds to sodium and pressure first
Urine albumin is one of the most diet-responsive kidney risk markers, especially through sodium and blood pressure. ACR below 30 mg/g is generally normal, 30–300 mg/g is moderately increased, and above 300 mg/g is severely increased.

When I see eGFR 72 mL/min/1.73 m² with ACR 420 mg/g, I do not call the kidneys “fine” just because creatinine is normal. Albuminuria predicts kidney and cardiovascular risk, and it often improves when sodium intake falls, blood pressure improves and diabetes treatment tightens.
Protein quantity matters, but protein source also matters. Plant-forward protein patterns may reduce acid load and improve blood pressure, while very high animal-protein diets can increase renal hemodynamic stress in susceptible patients; the effect size varies, and clinicians disagree on how strict to be in early CKD.
Serum albumin usually ranges from 3.5–5.0 g/dL, and low serum albumin with high urine protein can suggest significant urinary protein loss. Our low albumin guide explains why swelling, liver disease, inflammation and kidney loss need to be separated.
A practical trick: repeat ACR on a first-morning urine when possible. Exercise, fever, urinary infection, menstruation, severe hyperglycaemia and a very dilute sample can all make urine protein harder to interpret.
The DASH pattern can be kidney-friendly after modification
The DASH diet for blood pressure can help CKD patients, but standard DASH is not automatically safe for everyone with reduced eGFR. Its high fruit, vegetable, nut and legume content may raise potassium or phosphorus in patients who cannot excrete them well.

In early CKD with normal potassium, the DASH pattern often makes physiologic sense: lower sodium, more fibre, more unsaturated fats and better blood pressure. In CKD stage 4 with potassium 5.6 mmol/L, the same meal plan may need lower-potassium produce, smaller legume portions and avoidance of salt substitutes.
The thing is, DASH is a pattern, not a command to eat the highest-potassium foods daily. You can keep the sodium-lowering structure while choosing apples over orange juice, rice or pasta over potato, and unsalted fresh foods over phosphate-added packaged foods.
Patients with diabetes get an extra layer. If A1c is high, glucose control can reduce albuminuria risk, and our diabetes blood test guide explains why A1c, fasting glucose and kidney markers should be read together.
My usual test is boring but useful: change one dietary variable for 2–4 weeks, then recheck the lab most likely to move. If you change sodium, potassium, protein and supplements all at once, nobody can tell which lever helped.
Medicines can change what counts as a safe food
Kidney diet advice changes when medicines alter potassium, sodium, creatinine or acid-base balance. ACE inhibitors, ARBs, spironolactone, SGLT2 inhibitors, diuretics, NSAIDs, trimethoprim and phosphate binders can all change how food shows up in labs.

ACE inhibitors and ARBs can slightly raise creatinine after starting, often acceptable up to about 30% if potassium stays safe and the patient is clinically stable. That small creatinine rise may reflect lower intraglomerular pressure, which can be kidney-protective when albuminuria is present.
Spironolactone and eplerenone are where potassium food lists become more relevant. A patient eating high-potassium foods may do fine until a potassium-sparing drug is added; then a salt substitute with potassium chloride can push the lab from 4.8 to 6.1 mmol/L quickly.
NSAIDs are a quiet problem. Taking ibuprofen during dehydration, illness or heavy exercise can reduce kidney perfusion, raise creatinine and make an otherwise reasonable protein or sodium plan look harmful.
Supplements deserve the same respect as prescriptions. Our supplement timing guide covers interactions, and for kidney patients I specifically ask about creatine, magnesium, potassium, high-dose vitamin C, turmeric extracts and bodybuilding blends.
Repeat labs should be timed to answer one question
The best repeat kidney lab is timed around the specific diet change you made. BUN may change within days of protein adjustment, potassium can change within 24–72 hours after a major trigger, and ACR often needs several weeks of steadier blood pressure and sodium intake.

If creatinine is the concern, repeat after ordinary hydration, no intense exercise for 24–48 hours and no large cooked-meat meal the evening before. If potassium is the concern, repeat sooner after stopping potassium chloride salt or a risky supplement, especially when eGFR is below 45 mL/min/1.73 m².
For urine ACR, I like two out of three abnormal samples before making big claims, unless the value is very high or the clinical picture is obvious. ACR can swing with infection, exercise, fever, glucose spikes and even collection timing.
Kantesti AI reads trends across uploaded PDFs and photos, not just isolated highs and lows. Our blood test history tool helps patients see whether creatinine changed by 0.05 mg/dL noise or by a clinically meaningful slope.
Keep a simple 7-day note before repeat labs: protein grams if you track them, unusual restaurant meals, salt substitutes, supplements, workouts, diarrhoea, vomiting and new medicines. That note often explains the result faster than another expensive test.
Some lab patterns should not wait for diet experiments
Diet changes are not enough when kidney labs suggest urgent risk. Potassium of 6.0 mmol/L or higher, rapidly rising creatinine, severe acidosis, very low sodium, swelling with low albumin, or symptoms such as chest pain, confusion or severe weakness need medical advice quickly.

A creatinine rise of 0.3 mg/dL within 48 hours can meet acute kidney injury criteria in the right clinical setting. That is very different from a slow increase over several years, and it should not be managed by simply eating less protein.
Potassium symptoms can be vague or absent. I have seen patients with potassium 6.4 mmol/L feel “a bit tired” and nothing more, which is why high potassium gets taken seriously even when the person looks well.
Very low sodium is another trap. If sodium is below 130 mmol/L, drinking extra water because “kidneys need flushing” can make things worse; our low sodium guide explains why dilution, medicines and hormones must be sorted out.
Use diet as a long-game lever, not an emergency treatment. If a lab report says critical, or the patient has shortness of breath, fainting, chest symptoms, severe vomiting or new confusion, clinical care comes before food planning.
How Kantesti links kidney labs to food decisions
Kantesti connects kidney nutrition to the full lab pattern: eGFR, creatinine, BUN, electrolytes, CO2, calcium, phosphate, albumin and urine markers. Our AI does not tell every kidney patient to avoid the same foods; it looks for the constraint that actually shows up in the data.

Our platform can read a lab PDF or photo in about 60 seconds and translate the result into plain-language patterns. If you want to try it with your own kidney panel, use our free blood test analysis and include the urine ACR or urinalysis if you have it.
Kantesti AI interprets more than 15,000 biomarkers across blood chemistry, renal panels, urine markers, metabolic tests and micronutrients. For patients who want to understand marker names before uploading, our biomarker guide explains the abbreviations that commonly appear on kidney reports.
I still tell patients the same thing I say in clinic: AI interpretation is not a substitute for your nephrologist, primary care physician or renal dietitian. It is a way to catch patterns, prepare better questions and avoid the classic mistake of restricting potassium, protein or phosphorus without evidence.
Kantesti’s medical team is described on our medical advisory board, and the company background is available on About Kantesti. Thomas Klein, MD, reviews kidney-related content with the same bias I use clinically: protect the patient first, then optimize the numbers.
Research notes, validation and what we still do not know
The evidence for kidney diet is strongest for sodium reduction, blood pressure control, albuminuria reduction and supervised protein targets. The evidence is weaker for universal potassium restriction, aggressive phosphorus restriction in early CKD and supplement-based mineral correction without lab confirmation.
Kantesti LTD. (2026). Clinical Validation Framework v2.0. Zenodo. DOI link. Also available through ResearchGate search and Academia.edu search.
Kantesti LTD. (2026). AI Blood Test Analyzer: 2.5M Tests Analyzed | Global Health Report 2026. Zenodo. DOI link. Also available through ResearchGate record and Academia.edu record.
For a broader technical benchmark, our AI engine has also been evaluated in a pre-registered population-scale validation dataset across specialties; the methods are available in the AI engine benchmark. That does not remove uncertainty from kidney nutrition, but it does make the pattern-reading process auditable.
Bottom line from my side as Thomas Klein, MD: the best kidney diet is the one that improves the risky marker you actually have without creating a new one. If your potassium is normal, do not fear every vegetable; if your ACR is high, take sodium and blood pressure seriously; if phosphate is rising, hunt additives before cutting all nourishing foods, and use Kantesti AI blood test analyzer to track the pattern over time.
Frequently Asked Questions
What is the best diet for kidney disease based on blood tests?
The best diet for kidney disease depends on eGFR, urine ACR, potassium, phosphorus, bicarbonate, blood pressure, diabetes status and medications. A person with eGFR 72 mL/min/1.73 m² and ACR 250 mg/g may benefit most from sodium reduction and blood pressure control, while a person with eGFR 28 and potassium 5.8 mmol/L may need potassium restriction. Protein targets also differ: supervised non-dialysis CKD plans may use about 0.55–0.8 g/kg/day, while dialysis patients often need about 1.0–1.2 g/kg/day.
Can changing diet improve eGFR?
Diet does not usually raise true eGFR dramatically in a few days, but it can improve the risk markers around eGFR. Lower sodium can reduce blood pressure and urine albumin, avoiding dehydration can normalize a falsely high creatinine, and reducing excessive protein can lower BUN. If eGFR rises after stopping heavy exercise, cooked meat or creatine before testing, that may reflect cleaner measurement rather than kidney tissue repair.
Should everyone with kidney disease avoid foods high in potassium?
No, foods high in potassium should not be banned automatically in every person with kidney disease. Potassium usually ranges from 3.5–5.0 mmol/L, and restriction is most relevant when potassium is repeatedly above about 5.0–5.5 mmol/L, eGFR is low, or medicines such as ACE inhibitors, ARBs or spironolactone raise potassium risk. Whole-food potassium from fruits and vegetables is not the same as potassium chloride salt substitutes, which can raise potassium quickly.
Why did my BUN go up after eating more protein?
BUN rises when the body makes more urea from protein metabolism, so high-protein diets can raise BUN without an equal creatinine rise. Adult BUN is commonly about 7–20 mg/dL, though ranges vary by lab. A BUN-creatinine ratio above 20:1 often points toward dehydration, high protein intake, gastrointestinal nitrogen load or reduced kidney perfusion rather than kidney scarring by itself.
Is the DASH diet safe for kidney disease?
The DASH diet can be helpful for kidney disease when blood pressure is high, but it may need modification if potassium or phosphorus is elevated. The original DASH-Sodium trial showed systolic blood pressure reductions of about 7.1 mmHg in non-hypertensive adults and 11.5 mmHg in hypertensive adults when DASH eating was paired with low sodium. In CKD stage 4 or recurrent hyperkalemia, standard high-potassium DASH foods may need swapping for lower-potassium choices.
Which phosphorus foods matter most for kidney labs?
Phosphorus additives usually matter more than natural phosphorus in beans, nuts or whole grains because additive phosphorus may be absorbed at 90–100%. Serum phosphorus commonly ranges from 2.5–4.5 mg/dL, but PTH can rise before phosphorus becomes abnormal. Patients with CKD should look for ingredient words containing “phos” on packaged foods before cutting all nutritious plant proteins.
When should kidney lab results be treated as urgent?
Kidney-related lab results can be urgent when potassium is 6.0 mmol/L or higher, creatinine rises rapidly, sodium is very low, CO2 is severely low, or symptoms such as chest pain, fainting, confusion, severe weakness or shortness of breath occur. A creatinine rise of 0.3 mg/dL within 48 hours can meet acute kidney injury criteria in the right setting. Diet changes should not be used as the only response to critical kidney or electrolyte results.
Get AI-Powered Blood Test Analysis Today
Join over 2 million users worldwide who trust Kantesti for instant, accurate lab test analysis. Upload your blood test results and receive comprehensive interpretation of 15,000+ biomarkers in seconds.
📚 Referenced Research Publications
Klein, T., Mitchell, S., & Weber, H. (2026). Clinical Validation Framework v2.0 (Medical Validation Page). Kantesti AI Medical Research.
Klein, T., Mitchell, S., & Weber, H. (2026). AI Blood Test Analyzer: 2.5M Tests Analyzed | Global Health Report 2026. Kantesti AI Medical Research.
📖 External Medical References
KDIGO CKD Work Group (2024). KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney International.
📖 Continue Reading
Explore more expert-reviewed medical guides from the Kantesti medical team:

Diet for Fatty Liver: Food Choices That Move Labs
Fatty Liver Nutrition Lab Interpretation 2026 Update Patient-Friendly A practical, food-first guide to improving fatty liver lab trends...
Read Article →
Which Supplements Not to Take Together: Timing Guide
Supplement Timing Lab Interpretation 2026 Update Patient-Friendly Most supplement problems are not dangerous interactions; they are timing mistakes...
Read Article →
Magnesium Glycinate vs Citrate: Sleep, Stress, Labs
Supplements Lab Interpretation 2026 Update Patient-Friendly Glycinate usually fits sleep and stress goals; citrate is the practical choice...
Read Article →
Blood Tests for Fertility: Hormones Both Partners Need
Fertility Hormones Lab Interpretation 2026 Update Couple-Focused The most useful blood tests for fertility check ovulation, ovarian reserve,...
Read Article →
What Blood Tests Show Heart Problems? Marker Guide
Cardiology Markers Lab Interpretation 2026 Update Patient-Friendly Heart blood tests can point toward a heart attack, heart failure,...
Read Article →
What Blood Tests Should I Get for Easy Bruising?
Easy Bruising Coagulation Labs 2026 Update Patient-Friendly A symptom-first guide to the lab patterns doctors usually check when...
Read Article →Discover all our health guides and AI-powered blood test analysis tools at kantesti.net
⚕️ Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis and treatment decisions.
E-E-A-T Trust Signals
Experience
Physician-led clinical review of lab interpretation workflows.
Expertise
Laboratory medicine focus on how biomarkers behave in clinical context.
Authoritativeness
Written by Dr. Thomas Klein with review by Dr. Sarah Mitchell and Prof. Dr. Hans Weber.
Trustworthiness
Evidence-based interpretation with clear follow-up pathways to reduce alarm.