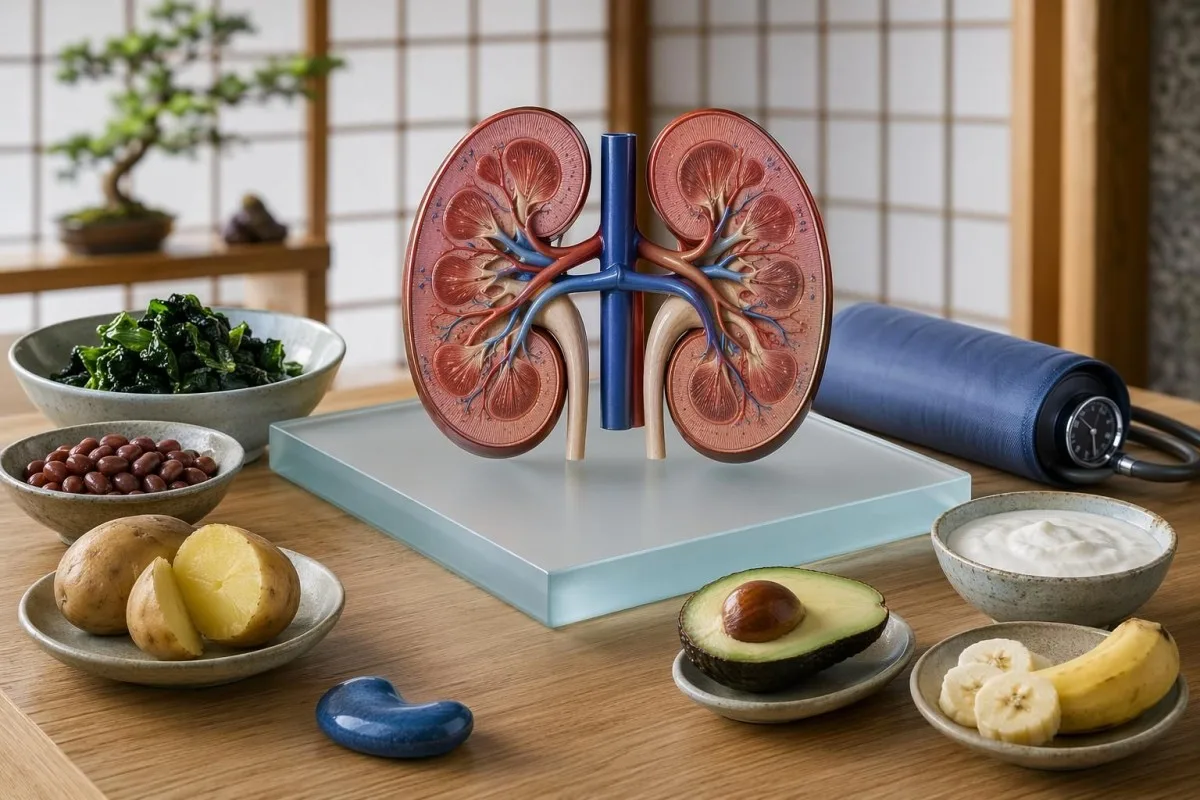
Potassium-rich foods can be excellent for blood pressure, but the same plate can be unsafe when eGFR, serum potassium, or certain medicines say otherwise.
This guide was written under the leadership of Dr. Thomas Klein, MD in collaboration with the Kantesti AI Medical Advisory Board, including contributions from Prof. Dr. Hans Weber and medical review by Dr. Sarah Mitchell, MD, PhD.

Thomas Klein, MD
Chief Medical Officer, Kantesti AI
Dr. Thomas Klein is a board-certified clinical hematologist and internist with over 15 years of experience in laboratory medicine and AI-assisted clinical analysis. As Chief Medical Officer at Kantesti AI, he leads clinical validation processes and oversees the medical accuracy of our 2.78 trillion parameter neural network. Dr. Klein has published extensively on biomarker interpretation and laboratory diagnostics in peer-reviewed medical journals.

Sarah Mitchell, MD, PhD
Chief Medical Advisor - Clinical Pathology & Internal Medicine
Dr. Sarah Mitchell is a board-certified clinical pathologist with over 18 years of experience in laboratory medicine and diagnostic analysis. She holds specialty certifications in clinical chemistry and has published extensively on biomarker panels and laboratory analysis in clinical practice.

Prof. Dr. Hans Weber, PhD
Professor of Laboratory Medicine & Clinical Biochemistry
Prof. Dr. Hans Weber brings 30+ years of expertise in clinical biochemistry, laboratory medicine, and biomarker research. Former President of the German Society for Clinical Chemistry, he specializes in diagnostic panel analysis, biomarker standardization, and AI-assisted laboratory medicine.
- Foods high in potassium include cooked beet greens at about 1300 mg per cup, Swiss chard at about 960 mg per cup, and a medium baked potato with skin at about 930 mg.
- Serum potassium is usually normal at 3.5-5.0 mmol/L in adults; values above 5.5 mmol/L deserve prompt review, especially with kidney disease or heart medicines.
- Blood pressure benefit is strongest when potassium intake rises while sodium intake falls; the DASH trial lowered systolic blood pressure by about 5.5 mmHg overall.
- Kidney safety changes when eGFR is below 60 mL/min/1.73 m², urine ACR is 30 mg/g or higher, or bicarbonate is low.
- Medication risk increases with ACE inhibitors, ARBs, spironolactone, eplerenone, trimethoprim, NSAIDs, tacrolimus, and potassium salt substitutes.
- High potassium diet is not the same as high serum potassium; most healthy kidneys excrete extra potassium within hours.
- False high potassium can happen after a difficult sample collection, prolonged tourniquet time, fist clenching, hemolysis, very high platelets, or very high white cells.
- Urgent potassium clue is a serum potassium of 6.0 mmol/L or higher, new weakness, chest symptoms, fainting, or an abnormal ECG pattern.
- CKD food strategy often means changing portions and preparation, not banning all vegetables; boiling and discarding water can lower potassium in potatoes and some greens.
Which foods high in potassium help blood pressure safely?
Foods high in potassium can help lower blood pressure when kidney function is normal and serum potassium is not elevated. The practical leaders are cooked beet greens, Swiss chard, potatoes with skin, acorn squash, spinach, lentils, beans, tomato paste, yogurt, avocado and bananas. A high potassium diet becomes risky when potassium is above 5.0 mmol/L, eGFR is below 60, urine ACR is high, or medicines reduce kidney potassium clearance.
As of May 13, 2026, I tell patients to treat potassium like a useful prescription-strength nutrient, not a wellness slogan. With Kantesti AI, our first check is not the banana count; it is the pattern across potassium, creatinine, eGFR, bicarbonate, glucose, and medication history.
The normal adult serum potassium range is about 3.5-5.0 mmol/L, although some laboratories flag 5.1 mmol/L while others wait until 5.3 mmol/L. A diet rich in potassium is usually safe when eGFR is 90 or higher, urine ACR is below 30 mg/g, and the patient is not taking potassium-retaining drugs.
I see a common mismatch: a 48-year-old with blood pressure around 146/88 mmHg adds lentils, yogurt, and spinach, then improves nicely; a 79-year-old on ramipril and spironolactone tries the same and returns with potassium at 5.8 mmol/L. If you already have a flagged result, read our normal potassium guide before changing your diet.
Ranked potassium-rich foods by realistic serving size
The highest potassium foods per common serving are usually cooked leafy greens, potatoes, beans, lentils, squash, tomato paste, yogurt, avocado, and dried fruit. Serving size matters more than food reputation: one cup of cooked beet greens can contain roughly three bananas worth of potassium.

Cooked foods often look smaller on the plate because water volume falls, so potassium becomes concentrated per cup. This is why cooked spinach can approach 840 mg per cup, while a casual handful of raw spinach contributes far less.
Bananas are not the champion. A medium banana has about 420 mg potassium, which is useful, but it is lower than a medium baked potato with skin, a cup of lentils, or a cup of cooked Swiss chard.
If your potassium is already high, avoid using internet food lists without checking your latest lab pattern. Our article on high potassium warning signs explains why the same food can be harmless for one person and risky for another.
How potassium lowers blood pressure in real physiology
Potassium lowers blood pressure mainly by increasing sodium excretion, relaxing blood vessel tone, and reducing the pressure effect of high salt intake. The effect is modest on average but clinically meaningful when baseline blood pressure is high or dietary sodium is excessive.

A BMJ meta-analysis by Aburto et al. found that increasing potassium intake reduced systolic blood pressure by about 3.49 mmHg and diastolic pressure by about 1.96 mmHg in adults, with stronger effects in people with hypertension (Aburto et al., 2013). That is not a medication-sized drop for everyone, but it is real.
The DASH trial by Appel et al. lowered systolic blood pressure by about 5.5 mmHg overall and about 11.4 mmHg in participants with hypertension using a diet rich in fruits, vegetables, and low-fat dairy (Appel et al., 1997). Potassium was one part of that pattern, along with magnesium, calcium, fiber, and less sodium.
The physiology is elegant. Higher potassium delivery to the kidney encourages natriuresis, meaning sodium leaves in the urine; for people comparing diet steps, our blood pressure range guide helps frame whether a 4-6 mmHg change is enough or needs medication support.
Who benefits most from a high potassium diet?
A high potassium diet tends to help most when blood pressure is above target, sodium intake is high, and kidney function is preserved. People with normal blood pressure may see little change, while people with salt-sensitive hypertension can see a more noticeable response.

In clinic, the clearest responders are often people eating restaurant meals most days, using packaged soups, or adding salt before tasting food. If sodium is still around 3500-5000 mg per day, potassium-rich foods may help but rarely solve the whole pressure problem.
The 2017 ACC/AHA hypertension guideline emphasizes dietary patterns, weight, sodium reduction, potassium-rich foods when safe, and regular activity rather than one isolated nutrient. For people adding supplements, our high blood pressure supplement guide covers the lab checks I want before magnesium, beetroot, or potassium products.
There is genuine uncertainty around individual cutoffs. Some patients improve with a potassium intake near 3000 mg/day, while others need a broader DASH-style pattern near 4000-4700 mg/day from food; I do not push those upper intakes if eGFR is falling or medicines are changing.
Kidney lab clues to check before increasing potassium
The kidney safety screen for potassium-rich foods is serum potassium, creatinine, eGFR, urine albumin-creatinine ratio, bicarbonate or CO2, and medication history. eGFR below 60 mL/min/1.73 m² or urine ACR of 30 mg/g or higher changes the conversation.
The KDIGO 2024 CKD guideline defines chronic kidney disease using reduced eGFR, markers of kidney damage such as albuminuria, or both for at least 3 months (KDIGO CKD Work Group, 2024). A single normal creatinine can miss early risk, especially in older adults or people with low muscle mass.
Urine ACR is underused. ACR below 30 mg/g is generally normal, 30-300 mg/g suggests moderately increased albuminuria, and above 300 mg/g signals higher kidney and cardiovascular risk; our urine ACR guide explains why albumin leakage often appears before creatinine rises.
Bicarbonate matters because metabolic acidosis can push potassium upward and often appears as low CO2 on a basic metabolic panel. When I review a CO2 of 18-21 mmol/L with eGFR 45 and potassium 5.2, I do not advise a spinach-and-bean challenge.
When a high potassium result is real or a lab artifact
A high serum potassium result can be real hyperkalemia or a false elevation from sample handling, hemolysis, prolonged tourniquet time, fist clenching, high platelets, or very high white cells. The first step is matching the number to symptoms, ECG findings, kidney function, and collection quality.

Serum potassium of 5.1-5.5 mmol/L is often mild, 5.6-6.0 mmol/L is more concerning, and 6.0 mmol/L or higher usually needs urgent clinical review unless clearly proven false. ECG changes or weakness make the number more serious at any level.
False highs are surprisingly common after a hard draw. If the lab reports hemolysis, or the potassium jumps from 4.3 to 5.9 mmol/L while creatinine and bicarbonate are unchanged, I usually repeat the test quickly before blaming beans, tomato paste, or bananas.
Kantesti's neural network flags inconsistent chemistry patterns, including potassium results that do not fit creatinine, CO2, sample comments, or prior trends. Our article on lab error checks gives examples of when a repeat sample is safer than a dietary overreaction.
Medications that make potassium-rich foods risky
Potassium-rich foods become riskier when medicines reduce aldosterone activity, kidney potassium excretion, or renal blood flow. The highest-risk combinations include ACE inhibitors or ARBs with spironolactone, eplerenone, trimethoprim, NSAIDs, or potassium salt substitutes.

ACE inhibitors such as lisinopril and ramipril, and ARBs such as losartan and valsartan, can raise potassium by lowering aldosterone signaling. Most patients tolerate them well, but risk rises when eGFR is below 60 or baseline potassium is already above 4.8 mmol/L.
Spironolactone and eplerenone are the medicines I watch most closely because they are designed to spare potassium. A patient can be stable at 4.6 mmol/L, then add a salt substitute and return at 6.1 mmol/L within days.
Trimethoprim can behave like a potassium-sparing diuretic at the kidney tubule, and NSAIDs can reduce renal perfusion during illness or dehydration. If a medication is new, use our medication monitoring timeline to see when potassium and creatinine commonly need rechecking.
How kidney disease changes potassium food choices
Kidney disease does not automatically mean zero potassium foods; it means potassium portions, preparation, and lab trends must guide the plan. In CKD stage 3 or higher, large servings of cooked greens, potatoes, tomato paste, dried fruit, and salt substitutes often need limits.

The old renal diet advice was often too blunt: avoid nearly every fruit and vegetable. In practice, a patient with eGFR 52, potassium 4.4, and ACR 18 mg/g may tolerate moderate potassium far better than someone with eGFR 28, potassium 5.3, and acidosis.
Boiling diced potatoes and discarding the water can lower potassium substantially compared with baking, though the exact drop depends on cut size, time, and water volume. Double boiling is sometimes used in renal nutrition, but it also strips flavor and water-soluble nutrients.
I prefer a food-by-food plan rather than a fear list. Our kidney disease diet guide gives a practical way to balance potassium, protein, phosphorus, sodium, and albuminuria instead of treating potassium as the only problem.
Diabetes, heart failure, and older adults need extra context
Diabetes, heart failure, and older age increase the chance that a potassium-rich diet will interact with kidney reserve, medicines, or dehydration. These groups can still benefit from foods to lower blood pressure, but their lab margin is narrower.

Diabetes can reduce kidney potassium excretion even before creatinine looks alarming, especially when albuminuria or type 4 renal tubular acidosis is present. I become cautious when potassium is 4.9-5.2 mmol/L plus CO2 is low-normal and ACR is rising.
Heart failure care often uses medicines that improve survival but raise potassium, including ACE inhibitors, ARBs, ARNIs, and mineralocorticoid receptor antagonists. A low-sodium, potassium-aware diet is usually safer than a blanket high-potassium diet in this group.
Older adults also have lower thirst reserve and more frequent illness-related dehydration. If glucose or A1c is part of the story, our diabetes blood test guide helps connect potassium risk with kidney, glucose, and medication patterns.
When low potassium is the bigger problem
Low potassium is usually more concerning than patients expect, especially with diuretics, vomiting, diarrhea, high aldosterone states, or poor intake. Serum potassium below 3.5 mmol/L can cause weakness, cramps, constipation, palpitations, and dangerous rhythm problems.

Thiazide and loop diuretics are common reasons a patient with hypertension becomes potassium-depleted. A potassium of 3.2 mmol/L on hydrochlorothiazide is not a trophy for avoiding bananas; it is a rhythm and muscle warning sign.
Low magnesium can make low potassium hard to correct because kidney tubules continue wasting potassium. I often check magnesium when potassium stays below 3.5 mmol/L despite food changes or prescribed replacement.
Patients sometimes restrict potassium after seeing one borderline lab and then feel worse. If your result is low or borderline low, our low potassium explainer covers the causes clinicians usually sort through first.
Salt substitutes and electrolyte drinks are not harmless
Potassium chloride salt substitutes and high-potassium electrolyte drinks can deliver medication-like potassium doses in small volumes. They are much riskier than eating a banana because the dose is concentrated and easy to repeat several times daily.

Some salt substitutes contain hundreds of milligrams of potassium in a small sprinkle, and a heavy-handed user can exceed 1000-2000 mg/day without noticing. That is the patient I worry about on lisinopril, spironolactone, or reduced eGFR.
Coconut water is another sneaky source. One cup may contain around 500-600 mg potassium, and two large bottles after exercise can rival several servings of high-potassium vegetables.
Palpitations after electrolyte products deserve a real lab check, not guesswork. Our irregular heartbeat lab guide explains why potassium, magnesium, calcium, TSH, and kidney markers often belong in the same review.
For a broader chemistry view, the electrolyte panel guide shows how sodium, potassium, chloride, and CO2 create patterns that single-result advice often misses.
How Kantesti AI reads potassium with kidney and diet context
Kantesti AI interprets potassium by comparing the result with kidney filtration, acid-base status, glucose, sodium, medications, prior results, and sample-quality clues. A potassium of 5.2 mmol/L means different things in a healthy runner than in a patient with CKD and spironolactone.
Our AI-powered blood test interpretation can read uploaded lab PDFs or photos in about 60 seconds and place potassium inside the full chemistry pattern. In our analysis of more than 2M blood tests from 127+ countries, isolated potassium flags often become clearer only after trend review.
Kantesti's clinical methodology is aligned with physician-reviewed safety rules, escalation thresholds, and lab-pattern checks. You can read more about our clinical standards if you want to see how we handle high-risk electrolyte findings.
We also map potassium against more than 15,000 biomarkers, including creatinine, eGFR, bicarbonate, magnesium, albumin, glucose, and urine ACR. The biomarker guide is useful when your report uses unfamiliar abbreviations or different units.
As Kantesti LTD, we are cautious about diet automation because kidney and medication context can turn good nutrition into harm. Thomas Klein, MD, reviews electrolyte content with that specific risk in mind.
Meal planning by potassium goal, not by food fear
Meal planning works best when potassium is matched to the goal: higher intake for blood pressure support, moderate intake for cautious kidney monitoring, or restricted intake during hyperkalemia risk. The same lentil bowl can be therapeutic, neutral, or unsafe depending on the lab pattern.

For blood pressure support with normal kidneys, I often start with one high-potassium food per meal: yogurt at breakfast, lentils at lunch, and squash or potatoes at dinner. That can add 1200-2000 mg/day without using powders or tablets.
For cautious kidney monitoring, I usually shift toward smaller portions: half a cup of beans instead of a full cup, boiled potatoes instead of baked, and tomato sauce used lightly. The goal may be 2000-3000 mg/day, but nephrology advice varies by CKD stage and serum potassium trend.
Food changes are easier to interpret if labs are repeated after the body has had time to respond. Our diet lab timeline guide explains which markers can change in days, weeks, or months.
Supplements are a separate category. If you are considering potassium, magnesium, beetroot, or multi-mineral products, our AI supplement recommendations are designed to consider labs first rather than guess from symptoms.
When to repeat labs or seek urgent care
Repeat potassium promptly when the result is unexpected, hemolysis is reported, medicines changed recently, or kidney markers shifted. Seek urgent care for potassium of 6.0 mmol/L or higher, fainting, severe weakness, chest symptoms, or suspected ECG changes.

If potassium is 5.1-5.5 mmol/L and you feel well, the next step is usually a repeat test, medication review, and kidney panel rather than panic. I still stop salt substitutes and potassium supplements while the result is being clarified.
If potassium is 5.6-6.0 mmol/L, I want faster follow-up, especially if eGFR is below 60 or a potassium-raising drug was started within the last 1-2 weeks. Our critical lab value guide explains why different labs call clinicians at different thresholds.
If symptoms appear, do not wait for a diet appointment. A telehealth blood test review can help triage mild cases, but chest pain, collapse, severe weakness, or potassium above 6.0 mmol/L belongs in urgent medical care.
Kantesti research, medical review, and next steps
The safest next step is to connect potassium-rich foods with your actual serum potassium, eGFR, urine ACR, CO2, and medication list. If those numbers are normal, potassium rich foods can be part of a blood-pressure plan; if they are not, the plan should be individualized.

You can upload your latest chemistry panel to Try Free AI Blood Test Analysis and get a structured interpretation in about 60 seconds. Kantesti AI does not replace your clinician, but it can make the next appointment more focused by showing which patterns deserve attention.
Our doctors and advisors review high-risk lab logic, including electrolyte thresholds, kidney patterns, and medication interactions. The Medical Advisory Board page explains the clinical oversight behind our patient-facing interpretation.
Kantesti LTD. (2026). Women's Health Guide: Ovulation, Menopause & Hormonal Symptoms. Figshare. DOI: 10.6084/m9.figshare.31830721. Research visibility: ResearchGate and Academia.edu.
Kantesti LTD. (2026). Clinical Validation of the Kantesti AI Engine (2.78T) on 100,000 Anonymised Blood Test Cases Across 127 Countries: A Pre-Registered, Rubric-Based, Population-Scale Benchmark Including Hyperdiagnosis Trap Cases — V11 Second Update. Figshare. DOI: 10.6084/m9.figshare.32095435. Research visibility: ResearchGate and Academia.edu.
Frequently Asked Questions
What foods are highest in potassium per serving?
The highest everyday foods high in potassium include cooked beet greens at about 1300 mg per cup, cooked Swiss chard at about 960 mg per cup, a medium baked potato with skin at about 930 mg, cooked acorn squash at about 890 mg per cup, and cooked spinach at about 840 mg per cup. Lentils, beans, tomato paste, yogurt, avocado, dried apricots, and bananas are also potassium rich foods. Serving size matters because cooked vegetables and concentrated tomato products can deliver far more potassium than people expect.
Can potassium-rich foods lower blood pressure?
Potassium-rich foods can lower blood pressure, especially when they replace salty processed foods and kidney function is normal. A BMJ meta-analysis found that increased potassium intake lowered systolic blood pressure by about 3.49 mmHg and diastolic pressure by about 1.96 mmHg in adults. The effect is usually stronger in people with hypertension, high sodium intake, or salt sensitivity.
When is a high potassium diet dangerous?
A high potassium diet can be dangerous when serum potassium is above 5.0 mmol/L, eGFR is below 60 mL/min/1.73 m², urine ACR is elevated, bicarbonate is low, or potassium-raising medicines are being used. ACE inhibitors, ARBs, spironolactone, eplerenone, trimethoprim, NSAIDs, tacrolimus, and potassium chloride salt substitutes raise the risk. Potassium of 6.0 mmol/L or higher needs urgent clinical review, especially with weakness, palpitations, chest symptoms, or ECG changes.
Is a banana enough potassium for blood pressure?
A medium banana contains about 420 mg of potassium, so it helps but is not enough by itself for a blood-pressure-focused diet. Many adults need a broader pattern with vegetables, beans, lentils, yogurt, potatoes or squash, lower sodium intake, and adequate magnesium and calcium. A single cup of cooked Swiss chard or a medium baked potato can contain more than twice the potassium of one banana.
What lab tests should I check before eating more potassium?
Before increasing potassium substantially, check serum potassium, creatinine, eGFR, urine albumin-creatinine ratio, CO2 or bicarbonate, glucose or A1c, and magnesium when symptoms or diuretics are involved. Serum potassium is usually normal at 3.5-5.0 mmol/L, and eGFR below 60 mL/min/1.73 m² reduces kidney potassium reserve. Urine ACR of 30 mg/g or higher suggests kidney stress even when creatinine looks acceptable.
Can a high potassium blood test be false?
Yes, potassium can be falsely high after hemolysis, prolonged tourniquet time, repeated fist clenching, delayed processing, very high platelets, or very high white blood cells. A sudden potassium jump from 4.3 to 5.8 mmol/L with stable creatinine and a hemolysis comment often deserves a prompt repeat sample. Symptoms, ECG findings, kidney function, and medication changes determine whether the result can wait or needs same-day care.
Are salt substitutes safe if I have high blood pressure?
Potassium chloride salt substitutes can lower sodium intake, but they are not automatically safe for high blood pressure. They may deliver hundreds or thousands of milligrams of potassium per day, which is risky with CKD, ACE inhibitors, ARBs, spironolactone, eplerenone, or baseline potassium above 4.8-5.0 mmol/L. Whole potassium-rich foods are usually safer than concentrated potassium products when labs and medicines are suitable.
Get AI-Powered Blood Test Analysis Today
Join over 2 million users worldwide who trust Kantesti for instant, accurate lab test analysis. Upload your blood test results and receive comprehensive interpretation of 15,000+ biomarkers in seconds.
📚 Referenced Research Publications
Klein, T., Mitchell, S., & Weber, H. (2026). Women's Health Guide: Ovulation, Menopause & Hormonal Symptoms. Kantesti AI Medical Research.
Klein, T., Mitchell, S., & Weber, H. (2026). Clinical Validation of the Kantesti AI Engine (2.78T) on 100,000 Anonymised Blood Test Cases Across 127 Countries: A Pre-Registered, Rubric-Based, Population-Scale Benchmark Including Hyperdiagnosis Trap Cases — V11 Second Update. Kantesti AI Medical Research.
📖 External Medical References
KDIGO CKD Work Group (2024). KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney International.
📖 Continue Reading
Explore more expert-reviewed medical guides from the Kantesti medical team:

Diet for Low Ferritin: Foods That Raise Iron Labs Safely
Iron Labs Nutrition 2026 Update Patient-Friendly Ferritin is not just an iron number; it is a storage signal...
Read Article →
Prebiotics Supplement: Gut Benefits and Lab Clues
Gut Health Lab Interpretation 2026 Update Patient-Friendly Prebiotics are not magic gut powder. Used carefully, they can shift...
Read Article →
NAC Supplement Benefits: Liver, Glutathione and Labs
Supplement Safety Liver Labs 2026 Update Patient-Friendly NAC is not a magic liver cleanse. Used thoughtfully, it can...
Read Article →
Vitamin D3 vs D2: Which Raises 25-OH Levels Best?
Vitamin D Lab Interpretation 2026 Update Patient-Friendly D3 usually raises and sustains 25-OH vitamin D better than D2,...
Read Article →
Magnesium Supplement Dosage: Labs, Forms and Safety
Magnesium Lab Interpretation 2026 Update Patient-Friendly A practical physician-written guide to choosing magnesium glycinate, citrate, oxide or food-first...
Read Article →
Pediatric Blood Test Normal Ranges by Age and Red Flags
Pediatrics Lab Interpretation 2026 Update Parent-Friendly Children’s lab results move with growth, puberty, feeding, infections, and even the...
Read Article →Discover all our health guides and AI-powered blood test analysis tools at kantesti.net
⚕️ Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis and treatment decisions.
E-E-A-T Trust Signals
Experience
Physician-led clinical review of lab interpretation workflows.
Expertise
Laboratory medicine focus on how biomarkers behave in clinical context.
Authoritativeness
Written by Dr. Thomas Klein with review by Dr. Sarah Mitchell and Prof. Dr. Hans Weber.
Trustworthiness
Evidence-based interpretation with clear follow-up pathways to reduce alarm.