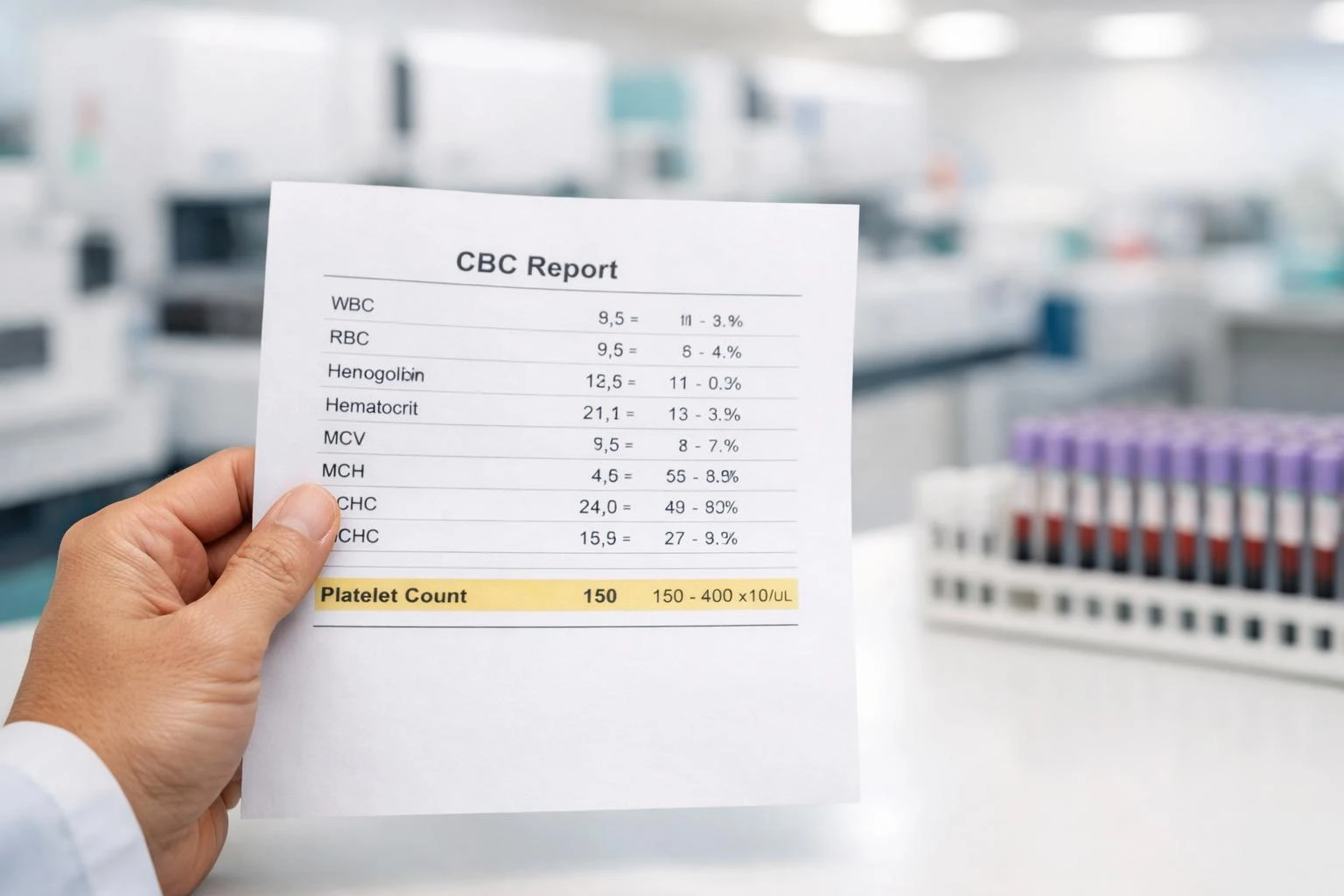
A CBC can look alarming when the platelet number falls outside range, but context usually changes the story. Here is how we interpret mildly high or low platelet results in clinic and inside Kantesti AI.
This guide was written under the leadership of Dr. Thomas Klein, MD in collaboration with the Kantesti AI Medical Advisory Board, including contributions from Prof. Dr. Hans Weber and medical review by Dr. Sarah Mitchell, MD, PhD.

Thomas Klein, MD
Chief Medical Officer, Kantesti AI
Dr. Thomas Klein is a board-certified clinical hematologist and internist with over 15 years of experience in laboratory medicine and AI-assisted clinical analysis. As Chief Medical Officer at Kantesti AI, he leads clinical validation processes and oversees the medical accuracy of our 2.78 trillion parameter neural network. Dr. Klein has published extensively on biomarker interpretation and laboratory diagnostics in peer-reviewed medical journals.

Sarah Mitchell, MD, PhD
Chief Medical Advisor - Clinical Pathology & Internal Medicine
Dr. Sarah Mitchell is a board-certified clinical pathologist with over 18 years of experience in laboratory medicine and diagnostic analysis. She holds specialty certifications in clinical chemistry and has published extensively on biomarker panels and laboratory analysis in clinical practice.

Prof. Dr. Hans Weber, PhD
Professor of Laboratory Medicine & Clinical Biochemistry
Prof. Dr. Hans Weber brings 30+ years of expertise in clinical biochemistry, laboratory medicine, and biomarker research. Former President of the German Society for Clinical Chemistry, he specializes in diagnostic panel analysis, biomarker standardization, and AI-assisted laboratory medicine.
- Platelet normal range for most adults is roughly 150,000 to 450,000 per microliter (150-450 x10^9/L).
- Low platelet count below 150,000/µL is called thrombocytopenia; bleeding risk usually rises much more once counts fall below 50,000/µL.
- High platelet count above 450,000/µL is called thrombocytosis; iron deficiency, inflammation, infection, and recovery after blood loss are common non-emergency causes.
- Critical low platelets below 10,000-20,000/µL can cause spontaneous bleeding and often need urgent medical assessment.
- Mild thrombocytopenia in the 100,000-149,000/µL range is often rechecked before major conclusions are drawn, especially if the rest of the CBC is normal.
- Mild thrombocytosis in the 451,000-600,000/µL range frequently reflects a reactive process rather than a bone marrow disorder.
- Platelet clumping in the tube can create a falsely low result; a repeat CBC in a citrate tube or a smear review can clarify this.
- Mean platelet volume (MPV) can add context, but platelet count matters more than MPV alone when deciding urgency.
- Red-flag symptoms include nosebleeds that do not stop, black stools, severe bruising, petechiae, chest pain, neurologic symptoms, or shortness of breath.
- Kantesti AI reviews platelet count alongside hemoglobin, white cells, iron markers, kidney function, and inflammatory patterns to explain whether a repeat test is reasonable.
What is the platelet count normal range on a CBC?
Platelet count normal range for most adults is 150,000 to 450,000 per microliter, written as 150-450 x10^9/L in many laboratories. A result slightly outside that band does not always mean disease — and some labs use narrower local ranges.

Platelets are small blood cell fragments that help blood clot after an injury. They are made in the bone marrow from megakaryocytes, circulate for about 7 to 10 days, and are then cleared mainly by the spleen and liver. When I review a CBC, the platelet count is rarely interpreted alone; hemoglobin, white blood cells, and the clinical picture matter just as much. If you want a broader refresher on CBC basics, our guide to reading blood test results covers the framework clinicians actually use.
The thing is, a reference range is not a hard border between healthy and unhealthy. A platelet count of 148,000/µL in a well person with a normal smear and stable prior tests can be less concerning than a sudden drop from 280,000 to 155,000/µL over a few weeks. Some European labs also report slightly different intervals based on analyzer method and population, which is one reason our AI on Kantesti AI looks at trends, not just one line item.
In our review of millions of uploaded lab panels, mild abnormalities are common and often temporary. A recent viral illness, heavy menstrual bleeding, dehydration, iron deficiency, recovery after surgery, and even lab artifact can nudge a platelet count up or down. That is why Kantesti AI ties platelet results to ferritin, CRP, kidney markers, and CBC indices rather than treating the number in isolation.
How labs report the same number differently
A platelet count of 250,000/µL is identical to 250 x10^9/L; only the units differ. Patients often think the values changed dramatically when they switched labs, but the count is the same once the units are translated.
Why platelets matter beyond just clotting
Platelets stop bleeding, but that is only part of the story. They also interact with the immune system, blood vessel lining, and inflammatory pathways, which helps explain why illness can push the count in either direction.

A normal platelet count supports primary hemostasis — the first step in sealing a damaged blood vessel. If platelets are very low, people can develop petechiae, easy bruising, gum bleeding, or prolonged nosebleeds. If platelets are very high, the concern is more complicated: many patients never develop symptoms, but clotting risk can rise in selected settings, especially when there is an underlying myeloproliferative disorder.
I see this pattern after infections all the time. A patient recovers from influenza or a bad gastrointestinal virus, feels better, and then the CBC shows platelets at 490,000/µL. That number often reflects the marrow 'rebounding' rather than anything dangerous. The practical move is usually to repeat the CBC after a few weeks, not to panic.
Platelets also need to be interpreted with coagulation testing when the story suggests bleeding or clotting. A platelet count can be normal while aPTT, fibrinogen, or D-dimer is abnormal, which is why readers with clotting concerns often benefit from our coagulation test guide. Kantesti AI uses that broader pattern recognition when users upload full reports.
What does a low platelet count mean?
Low platelet count means a result below 150,000/µL. The medical term is thrombocytopenia, and the urgency depends much more on the level, symptoms, and trend than on the word itself.

A platelet count of 100,000-149,000/µL is often called mild thrombocytopenia. Many people in this range have no symptoms and discover it incidentally during a routine CBC. If the rest of the blood count is normal and there is no bleeding, clinicians commonly repeat the test before launching an extensive workup.
Bleeding risk rises as platelets fall, but it is not linear and it is not identical for every person. Counts below 50,000/µL increase the chance of bleeding with trauma or procedures, and counts below 20,000/µL can lead to spontaneous mucosal or skin bleeding. A count below 10,000/µL is generally treated as a medical urgency because intracranial or gastrointestinal bleeding becomes a serious concern.
One of the most common misunderstandings is assuming every low result means an autoimmune disease. Sometimes it does — immune thrombocytopenia (ITP) is real — but just as often the explanation is medication effect, alcohol use, viral illness, liver disease with splenic enlargement, nutritional deficiency, pregnancy-related change, or pseudothrombocytopenia from platelet clumping in the tube. When anemia is also present, our iron studies guide and RDW article help fill in the missing context.
A practical clinic rule
If platelets are mildly low but hemoglobin, white cells, and smear are normal, observation and repeat testing often make sense. If platelets are low plus anemia, abnormal white cells, fever, neurologic symptoms, kidney injury, or active bleeding, the differential changes quickly and the threshold for urgent care drops.
What does a high platelet count mean?
High platelet count means a value above 450,000/µL. Most mild elevations are reactive thrombocytosis, not a bone marrow cancer — though persistent counts still deserve follow-up.

A platelet count of 451,000-600,000/µL is commonly seen after infection, surgery, blood loss, inflammation, or iron deficiency. This is the body's way of reacting to stress signals such as interleukin-6 and increased thrombopoietin activity. In daily practice, iron deficiency is one of the most underestimated causes — especially in patients with heavy periods, postpartum blood loss, or chronic gastrointestinal bleeding.
Here is a scenario I have seen more than once: a 34-year-old woman with fatigue and a platelet count of 525,000/µL worries about leukemia after reading her portal result. Her ferritin comes back 9 ng/mL, hemoglobin is borderline low, and the platelet elevation settles once iron stores improve. That is why a high platelet count paired with low MCV or abnormal RDW often pushes us toward iron studies first rather than the marrow.
Persistent counts above 600,000/µL, or any count that remains elevated for several months without an obvious trigger, need a more deliberate evaluation. If the platelet count reaches 1,000,000/µL, clinicians think more carefully about a myeloproliferative neoplasm such as essential thrombocythemia, particularly when there is headache, erythromelalgia, clotting history, or splenomegaly. Our platform connects these patterns with related markers and can be uploaded for review through our free blood test demo.
Common non-emergency causes of mild platelet abnormalities
Mild platelet changes are often caused by common, non-emergency conditions. The usual culprits are recent infection, iron deficiency, inflammation, alcohol use, medications, pregnancy, and lab artifact.

Recent viral illness can lower platelets for days to weeks, while recovery from infection can temporarily raise them. Alcohol can suppress marrow production and contribute to a low platelet count, especially when liver enzymes are also abnormal. Pregnancy adds its own version — gestational thrombocytopenia is usually mild, often appears in late pregnancy, and commonly stays above 100,000/µL.
Medications matter more than many people realize. Heparin can trigger heparin-induced thrombocytopenia, quinine can lower platelets, valproate can suppress counts, and some antibiotics do the same. On the other side, inflammation from autoimmune disease, rheumatoid arthritis, inflammatory bowel disease, or infection can create a high platelet count that improves once the underlying problem settles.
Lab artifact deserves respect because it fools people every week. EDTA-dependent platelet clumping can produce a falsely low result; a peripheral smear or repeat count in a citrate tube often solves the mystery. If the broader panel also hints at kidney disease, liver disease, or protein abnormalities, readers often find value in our BUN/creatinine ratio guide, eGFR article, and serum proteins guide.
When the count is mild and the patient feels well
A single platelet count of 138,000/µL or 472,000/µL in an otherwise well person is often rechecked rather than aggressively investigated on day one. This is one of those areas where context matters more than the number.
When should you repeat a platelet count?
Repeat testing matters when the platelet result is mildly abnormal, unexpected, or inconsistent with how you feel. A second CBC often separates temporary noise from a real trend.

For mild thrombocytopenia or thrombocytosis without symptoms, many clinicians repeat the CBC in 1 to 4 weeks, depending on the degree of change and the suspected cause. If the likely explanation is a recent infection, waiting 2 to 6 weeks can be reasonable. If the count is moving rapidly, or if you have bruising, bleeding, clotting symptoms, fever, or weight loss, the recheck interval is much shorter.
I often tell patients that trends beat snapshots. A platelet count that was 155,000/µL six months ago, 149,000/µL today, and 152,000/µL on repeat is a very different story from a drop from 310,000/µL to 149,000/µL in two weeks. Kantesti AI is particularly helpful here because our trend analysis flags whether a change is stable, progressive, or likely reactive.
Another reason to repeat quickly is suspected pseudothrombocytopenia. If the analyzer reports platelet clumps or the count seems oddly low in someone who has no bleeding history, a smear review and recollection can prevent unnecessary worry. You can upload a CBC PDF or photo to our platform or test the workflow first with the free demo.
Which platelet results are red flags and need urgent care?
Urgent care is more likely when the platelet count is very low, extremely high, or paired with dangerous symptoms. Numbers matter, but symptoms matter more.

A platelet count below 20,000/µL is a red flag, especially with gum bleeding, nosebleeds, blood in urine, black stools, heavy menstrual bleeding, or widespread petechiae. A count below 10,000/µL is particularly concerning for spontaneous bleeding even without trauma. These patients usually need same-day medical assessment.
Very high counts can also become urgent, although the pattern is less straightforward. Platelet counts above 1,000,000/µL can be associated with both clotting and bleeding because acquired von Willebrand dysfunction may develop at extreme levels. If the result is accompanied by chest pain, one-sided weakness, severe headache, visual change, or shortness of breath, do not wait for an online explanation.
The reason we worry about low platelets combined with anemia, kidney injury, or neurologic symptoms is that together they can suggest a thrombotic microangiopathy such as TTP, whereas an isolated mild low count is often much less dramatic. And if fever, abnormal white cells, and bruising appear together, hematology input becomes urgent. This is where our symptoms decoder and medical validation page help readers understand how our clinical logic is built.
How to interpret platelet count with the rest of the CBC
Platelet count becomes far more useful when read beside hemoglobin, white cells, MCV, RDW, and MPV. Patterns beat isolated values almost every time.

Low platelets plus low hemoglobin can point toward blood loss, marrow disorders, hemolysis, chronic liver disease, or nutritional deficiency, depending on the rest of the panel. High platelets plus low MCV or high RDW often points toward iron deficiency. That is why clinicians frequently connect platelet questions with ferritin, transferrin saturation, and red cell indices.
White cell changes add another layer. Thrombocytopenia plus leukopenia can occur with viral suppression, medications, or marrow disease; thrombocytosis plus neutrophilia often fits inflammation or infection. An abnormal smear can shift the picture again — giant platelets suggest increased turnover in some cases, while blasts or dysplastic cells point somewhere else entirely.
Kantesti AI was built for this kind of pattern recognition. Our neural network reads CBC markers alongside chemistry, inflammatory, and nutritional data in about a minute, which is especially useful when users upload prior reports for comparison. If you want the clinical scaffolding behind that approach, our blood test interpretation guide and medical advisory board page explain how we structure medical review.
What about MPV?
Mean platelet volume (MPV) estimates average platelet size. A high MPV can suggest increased marrow turnover in some settings, but MPV is too variable across analyzers to diagnose a cause by itself; the platelet count and smear remain more reliable.
How doctors think through the causes of low platelets
Doctors usually sort low platelet count into three buckets: decreased production, increased destruction, or sequestration in the spleen. That framework keeps the workup practical.

Decreased production happens when the marrow is not making enough platelets. Common reasons include alcohol-related marrow suppression, chemotherapy, vitamin B12 or folate deficiency, viral infections, aplastic anemia, and some bone marrow disorders. When several blood cell lines are low together, marrow production problems move higher on the list.
Increased destruction includes immune causes such as ITP, medication reactions, infections, and disorders like TTP or DIC. The pace matters here. A sudden fall in platelets over days is usually interpreted differently from a stable mild count that has looked the same for years.
Sequestration means platelets are being held in an enlarged spleen rather than truly absent from the bloodstream. Chronic liver disease and portal hypertension are classic examples. If liver enzymes, albumin, or coagulation markers are also off, the puzzle pieces start fitting together quickly.
How doctors think through the causes of high platelets
Doctors first decide whether a high platelet count is reactive or clonal. Reactive thrombocytosis is much more common, especially when the count is only mildly elevated.

Reactive causes include infection, inflammation, recent surgery, tissue injury, blood loss, iron deficiency, cancer, and recovery from thrombocytopenia. Platelet counts in these settings often normalize once the trigger resolves. A high CRP or ESR, low ferritin, or a recent medical event often tells the story before genetic testing is ever considered.
Clonal thrombocytosis is less common but clinically important. Essential thrombocythemia, polycythemia vera, and other myeloproliferative neoplasms may involve mutations such as JAK2, CALR, or MPL. Persistent platelet counts above 450,000/µL for more than 3 months, especially with splenomegaly or thrombosis history, usually prompt hematology review.
This is one of those areas where clinicians disagree on how aggressively to investigate modest elevations. Some prefer earlier mutation testing if the count remains above 600,000/µL without explanation; others lean harder on repeat CBCs and iron/inflammation workups first. In everyday outpatient medicine, the second approach is often more sensible.
Do normal platelet ranges differ in pregnancy, women, or older adults?
The usual platelet normal range stays close to 150,000-450,000/µL, but pregnancy and age can shift interpretation. Mildly lower counts are especially common late in pregnancy.

Pregnancy-related thrombocytopenia is often mild and typically stays above 100,000/µL. It is thought to reflect hemodilution, increased platelet consumption, and physiologic changes rather than disease in most cases. Counts below 100,000/µL, rising blood pressure, proteinuria, or abnormal liver tests raise a different conversation and can point toward preeclampsia or HELLP syndrome.
Women with heavy menstrual bleeding are also more likely to develop iron deficiency, which can push platelets upward rather than downward. That surprises people. If the CBC shows high platelets with microcytosis or fatigue, iron loss should be considered early, and our women's health guide often provides useful background.
Older adults can have slightly broader biologic variability, and medication lists tend to be longer. Aspirin, clopidogrel, anticoagulants, proton pump inhibitors, antiepileptics, and oncology drugs all complicate the picture. A borderline platelet count in an 80-year-old on multiple medicines needs a different lens than the same number in a healthy 25-year-old.
How Kantesti AI interprets platelet count results in context
Kantesti AI interprets platelet count by analyzing the CBC together with chemistry, iron status, inflammatory signals, symptoms, and prior trends. That mirrors how clinicians reason in real practice.

Our platform accepts blood test PDFs and photos, extracts the platelet count, standardizes units, and compares the value with age- and lab-aware reference logic. Then it looks sideways: hemoglobin, MCV, RDW, ferritin, CRP, creatinine, liver enzymes, and symptom inputs all help shape the interpretation. A mildly high platelet count with low ferritin reads very differently from the same platelet count with splenomegaly and recurrent thrombosis.
We built Kantesti AI to answer the question patients actually ask: 'Is this likely temporary, and what should I check next?' In many cases the best next step is not dramatic — it is a repeat CBC, iron studies, a smear review, or a medication review. Our About Us page and contact page explain how users, clinicians, and health partners use the service globally.
If you already have a CBC, the fastest way to see the full interpretation is to upload it to Kantesti AI or try the free blood test demo. The goal is clarity in under a minute, not generic reassurance.
Bottom line: when a platelet result is probably benign and when it is not
Most mild platelet count abnormalities are not emergencies. Persistent changes, severe out-of-range results, or any bleeding or clotting symptoms deserve quicker attention.

A platelet count of 135,000/µL after a viral illness or 480,000/µL during iron deficiency is often monitored and repeated rather than treated urgently. A count of 18,000/µL with nosebleeds, or 1,050,000/µL with neurologic symptoms, is a different category entirely. Context matters more than internet rules.
When I review platelet results, I am looking for pattern, pace, and partners — the other abnormal markers traveling with the platelet count. Is the number stable? Is the patient bleeding? Are kidney tests changing? Are there iron or inflammatory clues? Our AI blood test analyzer report shows how often trend analysis changes the interpretation.
So what does all this mean for you? If your platelet count is only mildly high or low and you feel well, repeat testing and context are often the right next steps. If symptoms are significant or the number is extreme, seek medical care promptly and let Kantesti AI help organize the lab picture while you do.
Frequently Asked Questions
What is a normal platelet count for adults?
A normal platelet count for most adults is 150,000 to 450,000 per microliter, which many labs write as 150-450 x10^9/L. Some laboratories use slightly different reference ranges based on their analyzer and local population data. A value just outside range does not automatically mean disease, especially if the result is stable and the rest of the CBC is normal. Clinicians usually interpret the number together with symptoms, prior trends, and other blood count markers.
How low does a platelet count have to be before it is dangerous?
Bleeding risk usually becomes more concerning when platelet count falls below 50,000/µL, especially before surgery, after injury, or with active bleeding. A count below 20,000/µL can cause spontaneous skin or mucosal bleeding, and a count below 10,000/µL is generally treated as a medical urgency. Danger also depends on medications, liver disease, infection, and whether anemia or clotting abnormalities are present. A mildly low count such as 120,000-149,000/µL is often monitored and repeated rather than treated as an emergency.
What causes a mildly high platelet count?
A mildly high platelet count, usually 451,000 to 600,000/µL, is most often caused by a reactive process rather than a bone marrow cancer. Common triggers include iron deficiency, recent infection, inflammation, surgery, blood loss, recovery after illness, and sometimes cancer-related inflammation. If ferritin is low or CRP is elevated, the platelet result often makes more sense. Persistent unexplained thrombocytosis, especially above 600,000/µL or lasting more than 3 months, usually needs additional evaluation.
Can dehydration affect platelet count?
Dehydration can mildly concentrate blood components and make some CBC values appear higher, including platelet count in selected cases. It is usually not the sole explanation for a major platelet abnormality, but it can contribute to borderline elevations. Repeating the test when you are well hydrated and no longer acutely ill can help clarify whether the result reflects physiology or a real hematologic pattern. This matters most when the initial result is only slightly above range.
Why would a platelet count need to be repeated?
A platelet count is commonly repeated when the result is only mildly abnormal, unexpected, or inconsistent with symptoms. Repeat testing helps identify temporary changes from infection, inflammation, blood loss, pregnancy, or medication effects, and it also catches lab artifacts such as platelet clumping. Many clinicians repeat a mild abnormal result in 1 to 4 weeks, although the interval changes with symptoms and severity. Trending is often more informative than a single isolated number.
Can iron deficiency cause high platelets?
Yes. Iron deficiency is a well-known cause of reactive thrombocytosis, and platelet counts can rise above 450,000/µL even when anemia is mild. This pattern is especially common in people with heavy menstrual bleeding, postpartum blood loss, or chronic gastrointestinal blood loss. When iron deficiency is treated and ferritin improves, the platelet count often drifts back toward normal. That is why high platelets plus low MCV or high RDW usually trigger iron studies.
What symptoms with abnormal platelets should prompt urgent medical care?
Urgent medical care is appropriate if an abnormal platelet count comes with ongoing nosebleeds, gum bleeding, black stools, blood in urine, severe bruising, widespread petechiae, chest pain, shortness of breath, severe headache, vision change, or one-sided weakness. These symptoms may signal active bleeding, clotting, or an underlying disorder that needs same-day assessment. Counts below 20,000/µL and counts above 1,000,000/µL deserve special caution, especially when symptoms are present. The urgency rises further if anemia, kidney injury, fever, or neurologic changes appear at the same time.
Get AI-Powered Blood Test Analysis Today
Join over 2 million users worldwide who trust Kantesti for instant, accurate lab test analysis. Upload your blood test results and receive comprehensive interpretation of 15,000+ biomarkers in seconds.
📚 Referenced Research Publications
Klein, T., Mitchell, S., & Weber, H. (2026). BUN/Creatinine Ratio Explained: Kidney Function Test Guide. Kantesti AI Medical Research.
Klein, T., Mitchell, S., & Weber, H. (2026). Urobilinogen in Urine Test: Complete Urinalysis Guide 2026. Kantesti AI Medical Research.
⚕️ Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis and treatment decisions.
E-E-A-T Trust Signals
Experience
Physician-led clinical review of lab interpretation workflows.
Expertise
Laboratory medicine focus on how biomarkers behave in clinical context.
Authoritativeness
Written by Dr. Thomas Klein with review by Dr. Sarah Mitchell and Prof. Dr. Hans Weber.
Trustworthiness
Evidence-based interpretation with clear follow-up pathways to reduce alarm.